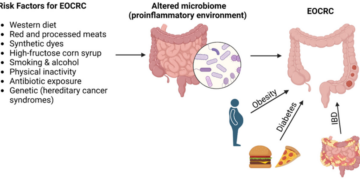
Diet
Cancer
Eyes
How Much Does Squint Eye Surgery Cost? A Complete Breakdown
Misaligned eyes can be fixed with squint eye surgery, also...
Read moreHow Does the Natural Eye See Light?
The natural eye is unequipped for separating individual frequencies yet...
Read moreThe Significance of Refreshing the Solution for Your Eyeglasses
Eyeglasses from an optometrist are a sound venture, with one...
Read moreExcercise
How In all actuality does Exercise Effect Rest?
There are many advantages to practicing routinelyConfided in SourceThe Workplace of Infection Anticipation and Wellbeing Advancement (ODPHP)The OODPHP assumes a...
Read more20 Excercise You Can Really do Frame Home
20 Excercise You Can In all actuality do Shape Home Standard activity is significant for keeping up with physical and...
Read moreAdhering to an Activity Program: 25 Hints to Make Exercise Progress
Adhering to a work-out routine is trying for essentially everybody, which is the reason it is fundamental to have proof...
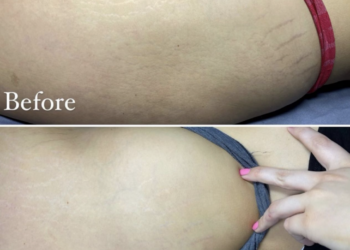
Read moreTummy Tuck vs Stretch Marks: Can a Tummy Tuck Procedure Remove Stretch Marks?”
Tummy Tuck vs Stretch Marks: Can a Tummy Tuck Procedure Remove Stretch Marks? If you have been considering a tummy...
Read moreBack Exercises that Build Muscle
Consistent, and progressive muscular training is the best way to increase muscle size(also known as hypertrophy) and strength). It’s also...
Read moreSkin
Stretch Marks
News

© 2023 HealthTopical - Premium WordPress news & magazine theme by HealthTopical.