Abstract
Telogen effluvium (TE) is the most common cause of diffuse hair loss in adult females. TE, along with female pattern hair loss (FPHL) and chronic telogen effluvium (CTE), accounts for the majority of diffuse alopecia cases. Abrupt, rapid, generalized shedding of normal club hairs, 2-3 months after a triggering event like parturition, high fever, major surgery, etc. indicates TE, while gradual diffuse hair loss with thinning of central scalp/widening of central parting line/frontotemporal recession indicates FPHL. Excessive, alarming diffuse shedding coming from a normal looking head with plenty of hairs and without an obvious cause is the hallmark of CTE, which is a distinct entity different from TE and FPHL. Apart from complete blood count and routine urine examination, levels of serum ferritin and T3, T4, and TSH should be checked in all cases of diffuse hair loss without a discernable cause, as iron deficiency and thyroid hormone disorders are the two common conditions often associated with diffuse hair loss, and most of the time, there are no apparent clinical features to suggest them. CTE is often confused with FPHL and can be reliably differentiated from it through biopsy which shows a normal histology in CTE and miniaturization with significant reduction of terminal to vellus hair ratio (T:V < 4:1) in FPHL. Repeated assurance, support, and explanation that the condition represents excessive shedding and not the actual loss of hairs, and it does not lead to baldness, are the guiding principles toward management of TE as well as CTE. TE is self limited and resolves in 3-6 months if the trigger is removed or treated, while the prognosis of CTE is less certain and may take 3-10 years for spontaneous resolution. Topical minoxidil 2% with or without antiandrogens, finestride, hair prosthesis, hair cosmetics, and hair surgery are the therapeutically available options for FPHL management.
Introduction
Women presenting with diffuse hair loss is a very common and challenging problem for dermatologists. The condition has several causes [Table – 1]. Telogen effluvium (TE) is the most common cause, followed by female pattern hair loss (FPHL) and chronic telogen effluvium (CTE); the rest of the causes are not so common and can be relatively easily diagnosed through history and examination. The problem arises in differentiating between TE, FPHL, and CTE, which account for the majority of diffuse alopecia cases in females. This article discusses the key diagnostic features and management strategies for these three most common causes of nonscarring diffuse hair loss in adult females.
Telogen Effluvium
First described by Kligman, TE is characterized by an abrupt onset, and rapid, diffuse, self-limited, excessive shedding of normal club hairs, usually seen 2-3 months after a triggering event. Among the various triggering events [Table – 2], the most common ones are severe febrile illness ( e.g. , malaria), postpartum (telogen gravidarum), accidental trauma, major surgery, emotional stress, chronic systemic illness, large hemorrhage, and crash diet. [1],[2],[3],[4] In one-third of cases, no trigger can be identified. Premature termination of anagen into catagen and telogen hair follicle is the main mechanism behind TE.
Acute TE or classical TE is a self-limiting condition lasting for about 3-6 months; however, if the stimulus/event that causes diffuse shedding persists beyond six months, then the condition becomes chronic. CTE is chronic diffuse loss persisting beyond six months, may be primary/idiopathic, or it may be secondary to some underlying disease and is described under the heading ′ chronic diffuse telogen hair loss ′ in the textbook of dermatology by Rook. The basic difference between chronic diffuse TE and classical TE is only that the stimulus which initiated the TE persists beyond six months and leads to chronicity. Among the various causes of chronic diffuse TE, iron deficiency anemia, hypo/hyper thyroidism, malnutrition, acrodermatitis enteropathica, and acquired zinc deficiency has been cited as the most widely accepted ones.
Diagnostic features of telogen effluvium
- Abrupt onset, rapid diffuse generalized shedding of hairs, usually seen 2-3 months after a triggering event. Nearly 100-1000 hairs/day may be lost.
- Strongly positive hair pull test. Usually more than 10% of the total hairs pulled are easily extracted from any part of the scalp in the acute phase of TE, if the patient has not shampooed the hairs for more than 24 hours. Approximately, 60 hairs are grasped between the thumb and the index and middle fingers and gently pulled. A negative test (≤6 hairs obtained) indicates normal shedding, whereas a positive test (>6 hairs obtained) indicates active hair shedding. [5],[6],[7]
- A trichogram (forcible complete hair pluck of 40-60 hairs) showing significant reduction in anagen:telogen ratio. [8] Usually,> 25% of the plucked hairs are telogen hairs in acute phase. No significant reduction in anagen:telogen ratio is seen in FPHL. Phototrichogram[9],[10] (all hairs within 2 sq cm area are trimmed 1 mm from the skin surface and photographed on day 1, day 3 or 4, and day 7 to assess the rate of hair growth, hair density, rate of shedding, etc.) and trichoscan[11] (fully computerized phototrichogram), are noninvasive, simpler, more reproducible, and sensitive techniques than classical trichogram, and are very useful in the diagnosis and management of hair loss.
- Videodermoscopy[12],[13],[14],[15] will show large number of short-tip pointed regrowing hairs in the absence of hair diameter variability.
- Biopsy shows normal histology except for an increase in the telogen follicles. The proportion of normal telogen follicles in excess of 15% is considered suggestive of TE. [2] while a level of 25% or more is considered definitive. Normal telogen counts are typically in the range of 6-13%. [16],[17] Biopsy, however, is not necessary for the diagnoses, but it does help to rule out FPHL and alopecia areata (AA).
- Differential diagnosis of TE generally includes FPHL, CTE, and rare cases of diffuse AA. The differentiating features of TE, FPHL, and CTE are enumerated in [Table – 3]. Abrupt onset diffuse AA with diffuse thinning and positive pull test may mimic TE, but the presence of exclamation point hairs, dystrophic hairs, circumscribed alopecia at other hair-bearing body areas, nail pitting, yellow dots on dermoscopy, and presence of peribulbar inflammatory lymphocytic infiltrate (swarm of bees) [18] clinches the diagnosis of AA. History and examination will generally suggest the cause of TE, and if not, then a minimum battery of laboratory tests, which includes complete blood count (CBC), routine urine, serum ferritin, and T3, T4, and TSH should be performed. [3],[19],[20] Iron deficiency anemia and thyroid hormone disorders are the two common conditions associated with TE and many a times, there are no apparent clinical features to suggest them, that is why they are included in the minimum battery of tests for cases of TE\diffuse alopecia with no apparent cause. [3],[19],[20],[21],[22],[23] If no cause is detected, then one must think of diffuse type of FPHL or CTE (idiopathic).
Female Pattern Hair Loss
FPHL is a gradual onset, slowly progressive nonscarring alopecia, which can be seen any time after menarche, but is most common in females aged 20-40 years. It results from a progressive reduction of successive hair cycle time leading to miniaturization of hair follicles. These changes are mediated through interaction between androgens, their respective receptors and enzymes like 5a reductase and p450 aromatase. [24],[25] Androgens definitely take part in the pathogenesis of the androgenetic alopecia in males, but their role in female alopecia is less certain and needs further investigation.
Three types of FPHL patterns have been described. [26]
- Diffuse central thinning (Ludwig type): The diffuse hair loss is concentrated over frontoparietal region leading to thinning/rarefaction over central scalp with intact frontal hair line [Figure – 1]. Ludwig graded it into three stages depending upon whether the central thinning is mild (stage I), moderate (stage II), or severe, that is, near-complete baldness of the crown (stage III).
- Frontal accentuation (Olsen type): It leads to widening of central parting line and thereafter to chrismas-tree pattern.
- Frontotemporal recession/vertex loss (male pattern/Hamilton type): It leads to recession of frontotemporal hairline or bitemporal recession and/or thinning at vertex.
The first two types are common and the third type is seen infrequently. The first type is often confused with CTE.
Hyperandrogenism is seen in < 40% of cases, [27] and may manifest through hirsutism, severe or recalcitrant acne, oligomenorrhea, infertility, acanthosis nigricans, and galactorrhea. Hormonal screening is indicated in cases with features of hyperandrogenism as well as in women in whom FPHL is abrupt, rapidly progressive, severe, or associated with severe bitemporal recession, to rule out any underlying cause for androgen excess like polycystic ovarian disease (PCOD), and ovarian or adrenal tumors. Minimum tests for hormones include total and free testosterone and/or dehydroepiandrosterone sulphate (DHEA-S). A more complete screening panel for hyperandrogenism consists of free and total testosterone, DHEA-S, LH, FSH, T3, T4, TSH, prolactin, and ultrasound for ovaries and adrenal glands. High levels of testosterones (2.5x normal or> 200 ng/dl) or DHEAS (>2x normal or> 700 µg/dl in premenopausal and> 400 µg/dl in menopausal women) should alert the physician to the possibility of androgen secreting tumor. [28]
Diagnostic features of female pattern hair loss
- Gradual onset, slowly progressive hair loss, which is often diffuse, and predominantly affects the frontoparietal region leading to central thinning with intact frontal hair line, or widening of central parting line. Rare cases may show frontotemporal or bitemporal recession with or without hair loss at vertex.
- Presence of miniaturized/vellus hairs (short thin hairs < 3 cm and a shaft diameter of £.03 mm) at the frontoparietal region is an important diagnostic feature of androgenetic alopecia. Vellus hairs along with bald scalp are, however, more common in males than in females and absolute bald area is not a feature of FPHL.
- Hair shaft diameter diversity, better seen during dermoscopy, is also a key feature of androgenetic alopecia. In addition, peripilar halos and peripilar atrophy can also be seen during dermoscopy in a few patients.
- Shedding may or may not be present, and if present, it is mild and never profound as noticed in TE/CTE.
- Hair pull test is usually negative.
- Histopathological examination reveals miniaturization of hair follicles, which is the histological hallmark of FPHL, and leads to significant reduction of terminal to vellus hair ratio. The T:V ratio is reduced from a normal of 8:1 to 2.2:1 in FPHL and any ratio < 4:1 is diagnostic of FPHL. [29] In addition, a slight increase in telogen hair count, 15-20%, predominantly lymphohistiocytic perifollicular infiltrate, perifollicular fibroses, and follicular streamers may also be seen. A horizontally, rather than vertically, sectioned 4-mm punch biopsy is more informative. [30]
- The main differential diagnosis of FPHL is CTE from which it needs to be differentiated [Table – 3].
Chronic Telogen Effluvium
First described by David A Whiting in 1996, CTE is an idiopathic distinct entity characterized by an excessive alarming diffuse shedding of hairs in females aged 30-60 years, with a prolong fluctuating course and near-normal histology. [31] The exact pathogenesis of CTE is not known, but it is theorized that it is due to reduction in the duration of anagen growth phase without miniaturization of hair follicles. Also, the etiology of CTE is unclear and it is diagnosed after excluding other causes of chronic diffuse hair loss.
Diagnostic features of chronic telogen effluvium
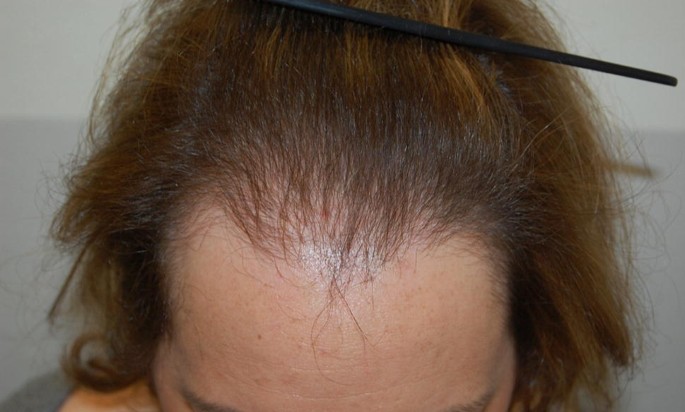
- History of abrupt, excessive, alarming, diffuse, generalized shedding of hair from a normal looking head is the main feature of CTE. Chunks of hair are seen in the bathroom (may block the drain), pillow, brush, and comb. Usually, a hand full of hair is displayed by the patient to corroborate the complaint of excessive shedding [Figure – 2].
- Obvious diffuse thinning is not a feature of CTE, though many of these women do notice 50% reduction in the volume of their ponytail thickness. Moderate to severe bitemporal recession may also be seen.
- A positive pull test at all sites of scalp (vertex, occipit, and sides) is seen in active phase.
- Absence of widening of central parting and miniaturization of hairs – the two features seen in FPHL.
- Absence of any underlying cause for chronic diffuse hair loss.
- Counting of total number of telogen hairs and vellus hairs (£– 3 cm) shed during standardized shampooing (wash test) has been reported as a good tool to differentiate between CTE and FPHL. [32] Ten percent or more of vellus hairs (£– 3 cm) is considered enough to diagnose FPHL.
- Normal histological picture except for a slight increase in the telogen hair follicles. For the purpose of differentiation from FPHL, a triple biopsy procedure in which three 4-mm punch biopsies had been taken simultaneously from the mid scalp was recommended. [33]
Management of Diffuse Hair Loss
A. General measures
- Identification and treatment of underlying cause: High fever, severe infection, or any other disease which could be the reason behind acute/chronic telogen hair loss should be identified and treated. Similarly, patients of FPHL with suspected androgen excess need hormonal assessment and treatment/referral to gynecologist/endocrinologist.
- Reassurance and explanation: The patient should be explained that TE or CTE represents excessive hair shedding rather than actual hair loss, all the hair lost would be replaced by regrowth and does not lead to baldness. It is a matter of time before the shedding stops. TE generally ceases within 3-6 months if the stimulus is removed, while CTE may take 3-10 years. Even in FPHL the picture is not gloomy. Baldness, unlike in males, is not a feature of FPHL. It only leads to thinning of hair, which can be prevented and to some extent regrowth of hair is possible through drugs like minoxidil.
- Assessment and treatment of iron deficiency and thyroid hormone disorders: The relationship between iron deficiency and hair loss have been recorded in several studies, [19],[34],[35],[36],[37],[38],[39],[40] some support the relationship of iron deficiency to TE, FPHL, CTE, and AA, while others do not. Currently, there is insufficient evidence to recommend universal screening for iron deficiency and to treat iron deficiency in patients of hair loss without anemia. Trost, Bergfeld, and Calogeras [19] have published an excellent review on the relationship and management of iron deficiency and hair loss. They practice screening for iron deficiency even in patients of hair loss without anemia and believe that the treatment of hair loss is enhanced when the serum ferritin concentration is raised to 70 µg/ml. For defining iron deficiency, different laboratories used different levels of serum ferritin ranging from 20-70 µg/ml, [35],[36],[37],[41] however, a cutoff below 41 µg/ml yields a sensitivity and specificity of 98%. [19],[42] Oral iron sulphate 300 mg (60 mg elemental iron) thrice daily may be given till a concentration of 70 µg/ml of serum ferritin is achieved and hemoglobin concentration, if low, is normalized. [43] Zinc and biotin have also been associated with hair loss, however, there are no concrete evidence to prove their role. [3] When no apparent cause is found, screening for T3,T4, and TSH is also recommended [22]
- Monthly assessment of the case: A resolving TE is characterized by absence of shedding, a negative hair pull test, and synchronized hair growth. Any unresolved TE with shedding of hairs beyond six months needs further evaluation, including a biopsy, to detect the underlying cause and to rule out FPHL. Patients of CTE and FPHL should also be kept under observation as wrong diagnosis of CTE in FPHL cases, simultaneous occurrence of CTE and FPHL, and chances of development of FPHL in CTE cases have all been reported. [32],[44] Numerous methods (biopsy, trichogram, unit area trichogram, phototrichogram, trichoscan, and videodermoscopy) are used to assess the hair growth variables (hair density, diameter, growth, anagen:telogen ratio, etc.) and to study the treatment response to various therapeutic modalities.
- Optimize the diet and avoid drugs associated with hair loss: The patient′s minimum intake should be 0.8 g/kg protein and at least 1200 Kcal per day. Vitamin A, vitamin A containing preparations like antioxidants, etetrinate, acitretin, and high dose OCP/HRT, etc. should be stopped or replaced with suitable substitutes. [20]
B. Specific treatment
1. Telogen effluvium
TE does not require specific drugs as the condition is self-limiting and usually resolves in 3-6 months if the trigger is removed. Complete recovery may take one year.
2. Female pattern hair loss [45]
- Minoxidil topical solution 2% – for mild to moderate FPHL (Ludwig stage I and II) without hyperandrogenism.
- Minoxidil 2% plus antiandrogens/finestride – for mild to moderate FPHL (Ludwig stage I and II) with hyperandrogenism.
- Hair prosthesis (wig, hair extension, hairpiece) and hair cosmetics (tinted powders, lotions sprays) – for severe FPHL (Ludwig stage III) and as adjuvant to medical therapy in mild to moderate cases. Severe cases do not respond to minoxidil and antiandrogens and surgery is not possible as the entire scalp including the donor area is susceptible and suffers from hair loss.
- Hair transplantation – ideal candidate for hair transplantation are moderate cases of FPHL (Ludwig stage II) who have high-density donor hair (>40 follicular unit/cm 2 ) in some areas and extensive loss or thinning at frontal or mid frontal scalp only. Women with mild FPHL (Ludwig stage I) are not optimal candidate as the difference between pre and post transplantation hairs is difficult to appreciate.
Minoxidil
Topical minoxidil has been shown to arrest hair loss and/or induce mild to moderate growth in approximately 60% of women with FPHL. [46] The beneficial effects of minoxidil lasts only till patient uses it. Minoxidil increases duration of anagen and enlarges miniaturized hair follicles by an unknown mechanism, which appears independent of its vasodilatory action. It is applied, at 1 ml twice daily to dry scalp, preferably through dropper. It takes approximately one hour for absorption, and before that if the hairs get wet, the process needs to be repeated. Minoxidil 2% (US FDA approved 2% for treatment of women with thinning of hairs) and 5% were found to be significantly more effective than placebo by both target area count and subjective assessment. [47] Target area count at 48 weeks showed a change, from baseline, of 24.5/cm 2 , 20.7/cm 2 , and 9.4/cm 2 in the 5%, 2% minoxidil, and placebo groups, respectively. This study did not show any significant difference between 2% and 5% minoxidil. In another well-designed 32 weeks study, 2% minoxidil stimulated mild to moderate growth in 63% of 157 women compared to 39% of 151 women treated with vehicle. [46] Results were less impressive in those with underlying hyperandrogenism. [48] Efficacy of minoxidil should not be judged before 6-12 months, although beneficial effects may be seen sooner.
Adverse effects of minoxidil are not common and includes irritation, hypertrichosis (7%) [49] over forehead and cheeks (avoid manual spread of minoxidil to sites other than scalp), which disappears within four months of stopping the treatment, allergic contact dermatitis, temporary self-limited shedding (telogen effluvium) of hair which begins at 2-8 weeks after treatment and subsides shortly with continued treatment. Minoxidil should not be used in pregnant and nursing mothers although no adverse pregnancy outcome were seen in a large scale one year prospective study. [50]
Antiandrogens
Antiandrogens may be beneficial, especially in cases of FPHL with hyperandrogenism. Although systematic antiandrogens, spironolactone (100-300 mg/day), [51],[52],[53],[54] flutamide (250-500 mg twice or thrice a day), [51],[55] and cyproterone acetate (CPA 100 mg/day on days 5-15 of menstrual cycle and ethinyl estradiol 50 µg/day on 5-25 days, or CPA 50 mg/day and ethinyl estradiol 35 µg/day on days 1-21 or a less effective combination of CPA 2 mg and ethinyl estradiol 50 µg) [56],[57] have shown some effectiveness in FPHL, none of these have been studied thoroughly in large placebo controlled trials. [20],[45] Presently, systemic antiandrogens can be tried (along with topical minoxidil) in FPHL with hyperandrogenism; however, their exact role can be defined only after studying their efficacy in the prospective placebo controlled trials. There is nothing to choose between different antiandrogens, the choice is personal. Since feminization of male fetus is a concern, concomitant use of oral contraceptive pill and pretreatment pregnancy test are mandatory in all females of childbearing age.
Finestride (1-1.25 mg/day) [58],[59],[60] is a potent 5a reductase (type II) inhibitor which blocks the conversion of testosterone to dehydrotestosterone (DTH). It is quite safe and does not require any blood test. DTH has a definitive role in the pathogenesis of androgenetic alopecia in males, so is the treatment with finestride. The role of DTH as well as of finestride in FPHL is, however, not very clear. In a well-controlled study, finestride 1 mg/day was not found to be useful in postmenopausal females, [59] while in another study, it has shown positive results in FPHL with hyperandrogonism. [58] Presently, it′s use is best reserved for patients of FPHL with hyperandrogenism.
3. Chronic telogen effluvium
There are no specific drugs for CTE. Empiric use of topical minoxidil 2% has been suggested in anticipation that it will prolong anagen growth. It is said that CTE is a self-limiting process, which may resolve spontaneously in 3-10 years, but there are no prospective long-term studies to substantiate these assertions. There is only one long-term study in which only five patients were followed up for seven years. [44] The natural history of CTE is poorly characterized and the prognosis is less certain.[61]
[“source=ijdvl”]
