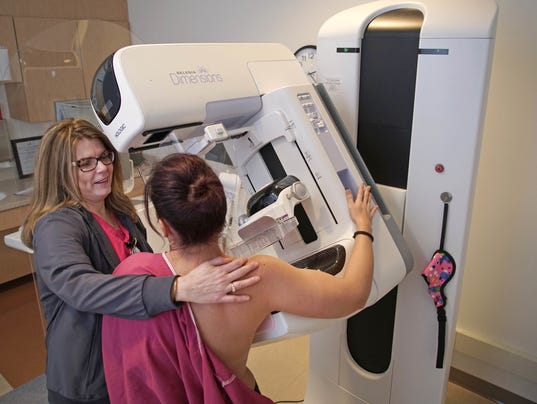
Starting this January, oncologists across the country will begin using new guidelines to describe the different stages of breast cancers.
The new rankings will now focus on the DNA of the tumor itself when determining the severity of the disease. The doctors hope the new system will allow for more precise treatment and avoid unnecessary chemotherapy for some women.
“In the long run it’s going to permit for better treatment,” said Dr. Rishi Sawhney, the medical director of the Bayhealth Cancer Institute in Dover.
The system should allow doctors to use drugs and treatments in a way more akin to a precise rifle shot rather than a shotgun blast that hopes to hit everything.
Doctors have been using the American Joint Committee on Cancer TNM system when diagnosing breast cancer. It was based on the size of the tumor, where the cancer had reached nearby lymph nodes and whether the cancer had metastasized (or spread).
More: Highmark’s Obamacare policies to rise 25 percent in Delaware
In that system, there are typically four stages of breast cancer, with the first stage meaning the cancer is contained in the breast and the fourth stage signifying that the cancer has spread to multiple other parts of the body. Stage IV breast cancer has been considered difficult to cure.
The new staging system will now add a fourth factor to the TNM system: Genomic testing, which will look at the DNA of the tumor.
“It comes from the realization that biology and genes of the tumor will trump everything else,” Sawhney said.
Genetic testing for things like the BRCA1 or BRCA2 gene can help predict the likelihood of a person getting breast cancer. Genomics, which is looking at how the genes in the tumor are working and interacting with other genes, can help determine whether the cancer will come back.
Read: Breast cancer awareness month calendar
Doctors will now use the Oncotype DX test to determine the woman’s genomic score. It takes a sample of the tumor and tests it for 21 genes. The test will analyze the likelihood of the breast cancer returning and the benefits of undergoing chemotherapy or radiation. (The same company makes tests for prostate and colon cancer patients).
The score ranges from 0-100, with a number higher than 31 indicating the need for a more aggressive course of treatment.
More than 170,000 patients have changed their breast cancer treatment decision because of the test, according to MyBreastCancerTreatment.org.
Women who might have previously been diagnosed at a Stage II might now be considered a Stage I, if they have a favorable Oncotype DX score, Sawhney said.
There is a difference between the Oncotype DX testing and testing for the BRCA gene, Sawhney pointed out. The BRCA gene is inherited.
Genomic testing, which is what the Oncotype test focuses on, only studies the genetic mutations of the tumor itelf. Those mutations aren’t hereditary. It examines a patient’s DNA for mutations in genes that make the patient more susceptible to the return of breast cancer.
The test is expected to be most helpful for women who are diagnosed with early-stage invasive breast cancer or DCIS (non-invasive) breast cancer.
More: This man believes rowing could make Wilmington healthier — and safer
Sawhney doesn’t anticipate that women who have already been diagnosed with breast cancer before the guidelines go into effect will be re-diagnosed in January. They are likely to already be receiving some type of treatment, he said.
Re-diagnosing women and deciding how to then proceed with treatment could become “very muddled,” he said.
Sawhney expects the new staging guidelines will quickly become the standard for doctors both in the U.S. and all over the world. Using molecular features to assign a stage will better identify aggressive cancer and spare some from undergoing intense treatment.
“We’ll be more cutting edge,” he said.
Source:-delawareonline

